Now Reading: Report: US Health Funding Cuts Threaten Your Access to Quality Health Care
-
01
Report: US Health Funding Cuts Threaten Your Access to Quality Health Care
Report: US Health Funding Cuts Threaten Your Access to Quality Health Care
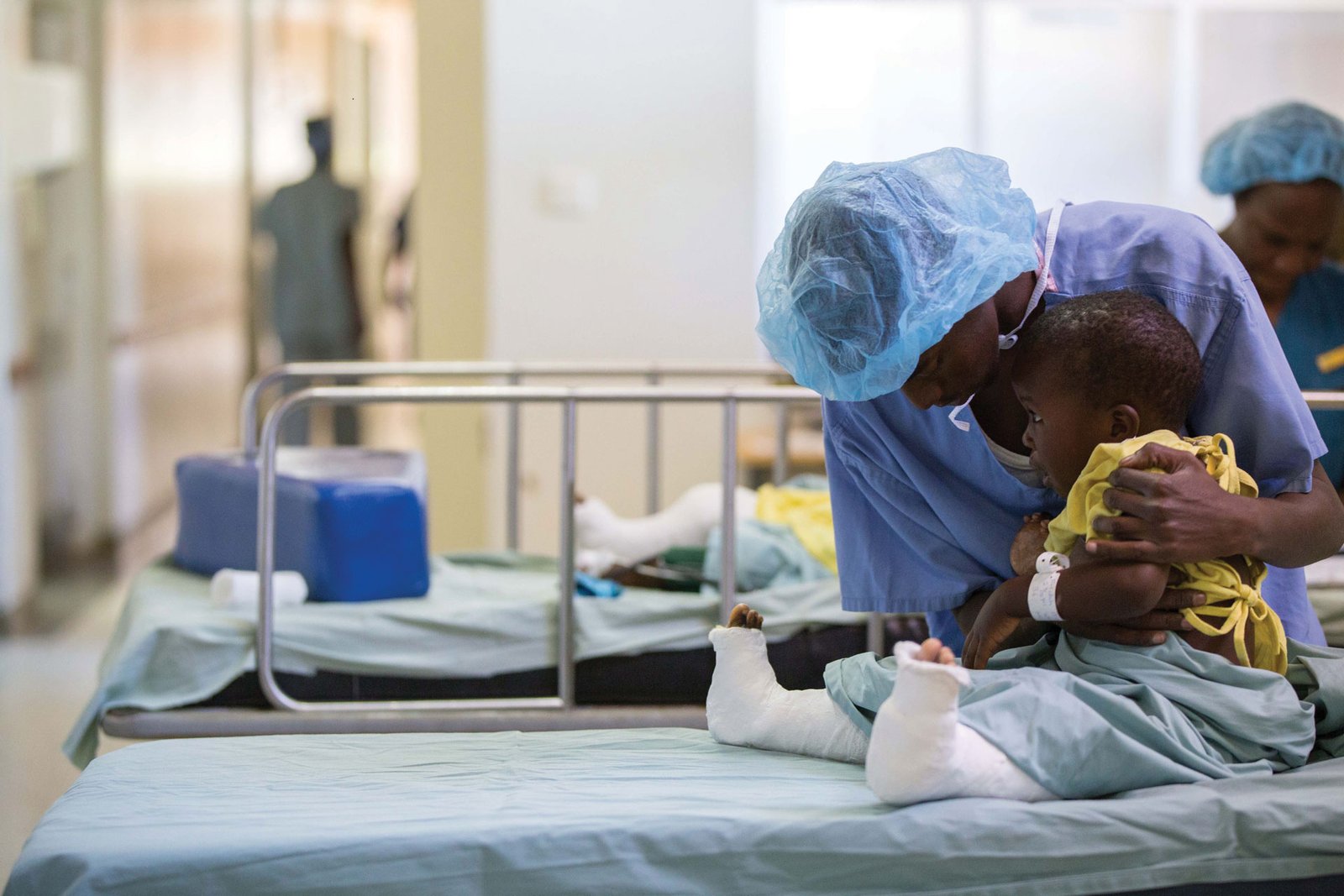
The sweeping cuts to U.S. global health funding has left Kenya facing a Sh34.7 billion healthcare shortfall, disrupting HIV, malaria, maternal, and child health services, as well as essential medicines and immunizations, and putting ordinary Kenyans, especially pregnant women, children, and adolescents, at serious risk.
A recent report by The Centre for Epidemiological Modelling and Analysis (CEMA) at the University of Nairobi warns that the abrupt withdrawal of external support has left hospitals struggling to maintain services, health workers uncertain about their jobs, and vulnerable populations at heightened risk of disease.
From 2020 to 2025, the United States provided approximately $2.5 billion in foreign aid to Kenya, with 80 percent dedicated to health programs.
In January 2025, a U.S. executive order paused foreign assistance for review, followed by legislative cuts confirmed in July. The result of which is a severe shortfall in resources without any immediate alternative funding.
For everyday Kenyans, the health care consequences are tangible
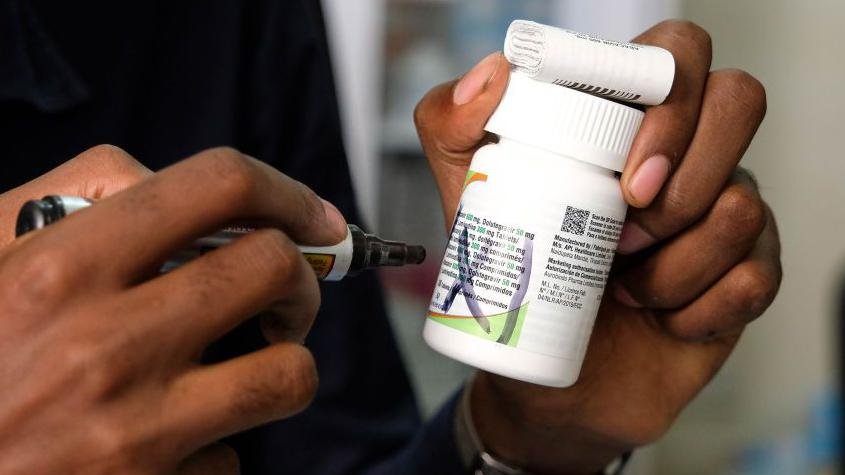
Drop-in centers for HIV testing and prevention, largely funded through the U.S.-backed PEPFAR program, have been abruptly suspended.
Approximately 41,500 health workers, nearly one-fifth of the nation’s healthcare workforce, were supported by U.S. funds, many of whom now face layoffs or redeployment.
Antiretroviral therapy clinics have temporarily closed, leaving patients scrambling for alternatives, while programs that offered HIV counseling and pre-exposure prophylaxis for adolescent girls and key populations have been halted.
“These cuts are reversing years of progress,” says Dr. David Khaoya, lead author of the CEMA report. “Young women who were part of the DREAMS initiative, designed to keep them HIV-free, are now forced to make risky choices to survive. Communities that relied on preventive health services are suddenly left without support.”
Malaria net distribution, maternal and child health programs, routine immunizations, and nutrition initiatives have also been disrupted.
Parents now face longer waits at clinics, shortages of essential medicines, and the threat of resurgent diseases such as malaria, measles, and polio.
Vaccine-preventable diseases are particularly alarming, as the withdrawal of U.S. support for Gavi, the global vaccine alliance, compounds an ongoing crisis that has already left thousands of children vulnerable.
The report notes a Sh34.7 billion funding gap in Kenya’s healthcare system. Counties must absorb the salaries of 41,170 PEPFAR-supported health workers, mostly deployed in high HIV-burden areas, putting further strain on limited domestic resources.
Health information systems, critical for disease monitoring and outbreak response, are also under threat, making it harder to track progress or identify emerging health emergencies.
For ordinary citizens, the cuts mean more than empty shelves at clinics. Pregnant women risk losing access to essential prenatal care, children face interruptions in immunization schedules, and communities could see spikes in HIV and TB infections.
Adolescents, particularly girls and young women, are disproportionately affected, widening already existing inequities in access to care.
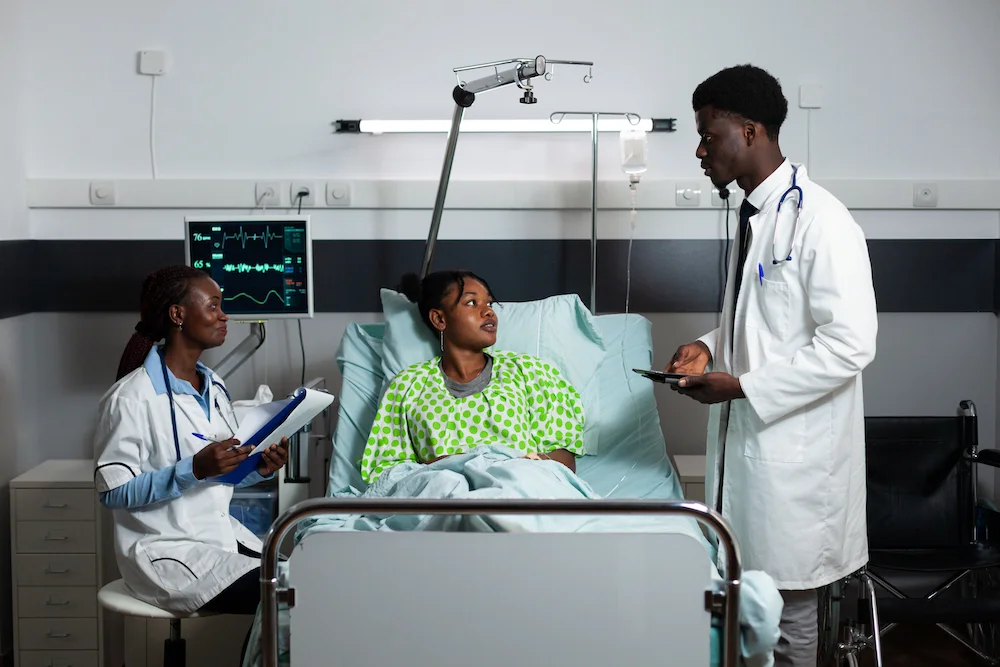
Yet the report argues the crisis also offers an opportunity for Kenya to rethink its health financing. Dr. Khaoya stresses the need to increase domestic investment, strengthen national ownership, and reduce overreliance on external aid. “While this funding shock poses serious risks, it is also a call to build a self-reliant and resilient health system,” he says.
Health officials warn that without immediate intervention, ordinary Kenyans may experience longer-term health consequences.
As families navigate rising costs, closed clinics, and limited access to lifesaving medicines, the gap left by U.S. funding exposes how heavily Kenya has relied on external support, and how urgent the need is for a more sustainable, locally driven health system.
Also Read: Hospital M&A Declined in 2025 Amid Policy Uncertainty, Financial Stress – Business News





